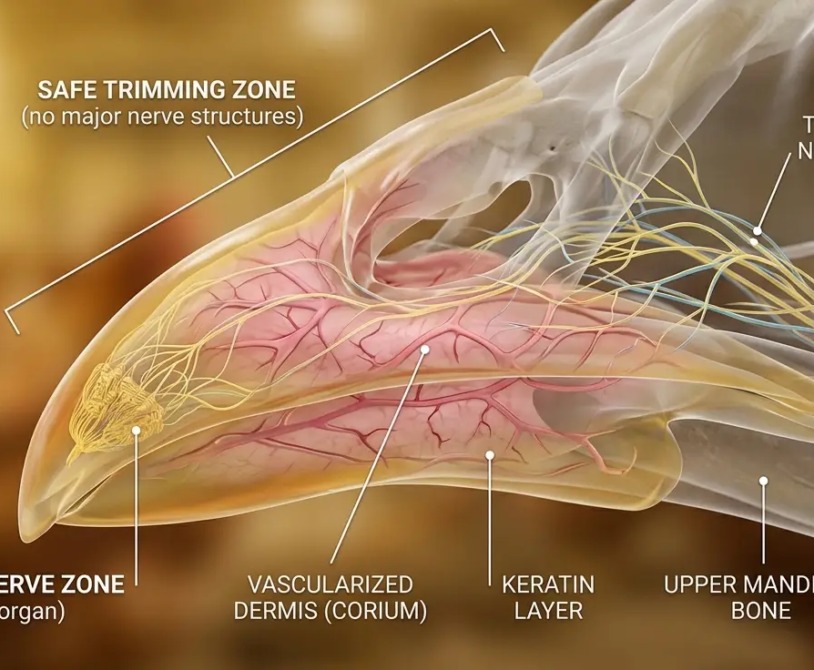
A sick hen is a question. The farm diagnosis tool is the method for answering it.
The question is never simply “what disease is this?” The question is: what combination of signs, history, and environmental context is present in this flock, and what do those signs — taken together, in sequence, at this age and production stage — point toward as the most likely cause? And then: what do I do with that answer in the next 6 hours?
Most farm-level diagnostic mistakes are made not because the farmer lacks knowledge of the diseases, but because the diagnostic process is disordered — one sign is observed, a conclusion is reached, and treatment begins before the other signs that would have revised the conclusion are examined. A hen with green diarrhea gets treated for Newcastle disease before anyone counts the mortality rate, checks the vaccination record, or opens a dead bird. The mortality rate is 0.05% per day (not NDV), the vaccination record is current, and the necropsy reveals Marek’s Disease lymphoma in the viscera. Three days and a treatment course were wasted because the diagnostic process stopped at the first sign.
This article builds a structured farm diagnosis framework — a sequence of observations that generates a differential diagnosis list, a necropsy protocol that narrows it, and a decision tree that converts the clinical picture into a management action before laboratory confirmation arrives.
The Diagnostic Framework: Five Stages in Order
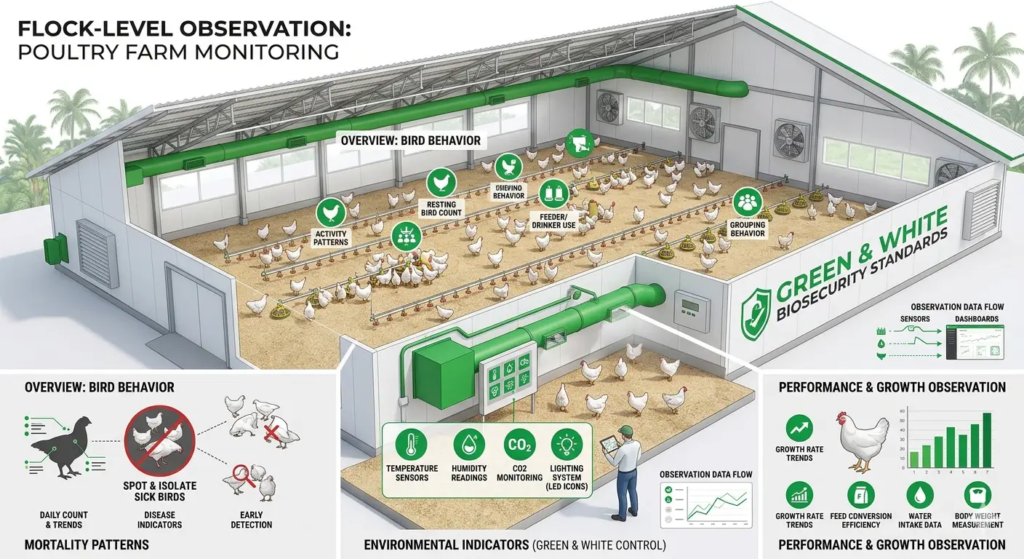
Stage 1 — Flock-Level Observation (Before Touching a Bird)
The first stage of farm diagnosis requires no equipment and no physical bird handling. It requires standing in the house and observing systematically before forming any hypothesis.
Walk the full length of the house. Observe from the center. Record the following before approaching any individual bird:
Mortality pattern:
- How many dead birds are visible?
- Where are the dead birds located in the house — distributed evenly, clustered at one end, concentrated in specific cage rows or floor zones?
- What is the posture of dead birds — sudden death (normal posture, no evidence of distress), or found after a period of illness (lateral recumbency, signs of struggling)?
- What is the daily mortality count compared to the previous 3 days? Rising, stable, or falling?
Behavioral pattern of living birds:
- What percentage of the flock appears normal versus showing abnormal behavior?
- What specific abnormal behaviors are visible: huddling, ruffled feathers, sitting on hocks, torticollis, labored breathing, extended neck posture, circling, wing droop, unilateral lameness, isolation from the flock, vent pecking?
- Are affected birds distributed evenly across the house or concentrated in a specific area or age group?
Production indicators:
- What is today’s egg count compared to the breed standard for the current age?
- Are there more floor eggs than usual?
- Are there more soft-shelled or shell-less eggs in today’s collection than in the previous week?
Environmental indicators:
- What is the ammonia level (estimated by smell, or measured with an ammonia meter if available)?
- What is the litter condition — dry, moist, wet patches?
- What is the house temperature relative to the target for the current age and season?
- Is the ventilation system operating normally?
Record all observations before moving to Stage 2. The behavioral patterns and production indicators visible at the flock level often generate a shorter differential list than any individual bird examination.
Stage 2 — Individual Bird Examination (The Clinical Assessment)
Select 5–10 birds for individual examination: include 2–3 that appear most severely affected, 2–3 that appear mildly affected, and 2–3 that appear clinically normal from the same flock section. Examining only the most affected birds gives a partial picture; examining apparently normal birds alongside them reveals whether subclinical signs are present across the flock.
Examine each bird systematically, in the same sequence every time:
1. General appearance:
- Body condition: Is the keel bone prominent (underweight)? Is there adequate breast muscle coverage?
- Hydration: Are the skin folds over the hock joint elastic and moist (well-hydrated) or dry and non-elastic (dehydrated)?
- Feather condition: Normal gloss, or dull and ruffled?
- Eye brightness: Clear and alert, or dull and sunken?
2. Head and neck:
- Comb and wattles: Size and color relative to expected stage of lay (bright red = reproductively active; pale and shrunken = reproductively suppressed or anemic)
- Nasal discharge: Absent, serous (clear and watery), or mucopurulent (thick and cloudy)?
- Ocular discharge: Absent, serous, or mucopurulent?
- Facial swelling: Absent or present? If present, bilateral (both infraorbital sinuses — infectious coryza, Mycoplasma) or unilateral?
- Tracheal sounds: Listen with ear near the bird’s open beak — are there clicking or rattling sounds indicating fluid or exudate in the trachea?
3. Respiratory assessment:
- Respiratory rate: Normal (12–25 breaths per minute at rest) or elevated?
- Pattern: Normal bilateral chest movement, or labored with exaggerated abdominal lift?
- Open-mouth breathing (gasping): Indicates severe respiratory compromise — upper respiratory obstruction, severe pneumonia, or heat stress
4. Abdominal palpation:
- Normal: Soft, compressible abdomen with no abnormal masses
- Fluid-filled pendulous abdomen: Egg peritonitis, ascites (water belly from right ventricular failure), or fatty liver hemorrhage syndrome
- Hard masses in the lower abdomen: Impacted egg, ovarian tumor, Marek’s disease lymphoma
5. Vent examination:
- Vent appearance: Moist, pink, and normally sized (productive hen) or dry, pale, and shrunken (non-laying)
- Pasting or soiling: Dried fecal material around the vent feathers — indicates diarrhea, which is not a specific diagnosis but narrows the differential
- Prolapse: Visible protrusion of oviduct tissue through the vent — requires immediate isolation of the affected bird to prevent cannibalism
6. Droppings assessment: Examine fresh droppings from the cage pan or litter beneath where affected birds are housed. Normal droppings: formed, brown-green with white urate cap. Abnormal droppings and their significance:
| Dropping Appearance | Possible Cause |
|---|---|
| Green and watery | Newcastle disease, Marek’s (liver involvement), starvation |
| Yellow-orange and watery | Infectious Bursal Disease, liver dysfunction |
| White and watery (rice-water) | Infectious Bronchitis (nephropathogenic strain), Infectious Laryngotracheitis |
| Blood-tinged | Coccidiosis, hemorrhagic enteritis, Clostridium perfringens necrotic enteritis |
| Grossly bloody | Severe coccidiosis, hemorrhagic bowel syndrome |
| Brown and foamy | Cecal coccidiosis (Eimeria necatrix or E. tenella) |
| Excess cecal droppings (dark, malodorous) | Normal (cecal droppings occur 1–2× daily) — do not over-interpret unless all droppings are cecal-type |
Stage 3 — Mortality History and Production Context
The clinical examination of individual birds must be interpreted in the context of the flock’s production history and recent management events. This context determines whether a sign is a primary disease event or a secondary complication.
The 14-day review:
Before reaching any diagnostic conclusion, answer these questions about the previous 14 days:
- What vaccinations were administered, on which days, and by which route?
- Were there any ration changes — ingredient source, formula, or feed supplier?
- Were there any management changes — stocking density, lighting program, feeding system?
- Were any new birds introduced to the farm?
- Did any visitors enter the production area who had previously been on another poultry farm, at a live bird market, or in contact with backyard poultry?
- Was there a power outage or lighting disruption?
- Was there a significant temperature event — a heatwave, an unusual cold night during harmattan season?
- Was there a water supply interruption or water quality change?
Many disease presentations that appear as primary infectious events are actually secondary consequences of a management event that occurred 7–14 days earlier. Respiratory disease presenting at day 21 may be the consequence of a Gumboro vaccination that was administered during the maternal antibody window at day 16 and produced immunosuppression rather than immunity. An egg drop presenting at week 22 may be the consequence of a lighting disruption at week 20. The 14-day review creates the timeline that places the clinical signs in their management context.
Stage 4 — Field Necropsy Protocol
Necropsy — systematic examination of a dead or euthanized bird — is the most information-dense diagnostic action available at the farm level. It takes 10–15 minutes per bird when performed correctly, requires no specialized equipment beyond a sharp knife or scissors, and produces a set of gross pathology findings that — interpreted alongside the clinical picture from Stages 1–3 — narrows the differential diagnosis list in most cases to 1–3 candidates.
Necropsy must be performed on fresh birds. A bird dead for more than 4 hours at ambient tropical temperatures shows autolytic changes — organ color changes, gas accumulation, tissue softening — that confound interpretation. Submit the freshest possible carcasses or euthanize moribund birds immediately before necropsy.
The systematic necropsy sequence:
External examination:
- Feather condition, body condition score, vent soiling, skin lesions
- Look for: Marek’s disease peripheral nerve enlargement (sciatic nerve — visible through the skin at the base of the thigh; an enlarged sciatic nerve larger than normal is a Marek’s disease finding), skin tumors, external parasite presence (check vent area, under wings)
Subcutaneous and crop:
- Open the skin from the keel to the beak along the midline
- Examine the crop: Empty (feed deprivation or anorexia), full and normal, or impacted (pendulous crop from water deprivation then gorging, or Candida ingluvitis)
- Examine subcutaneous fat: Normal (pale yellow), absent (cachexia), or gelatinous and edematous (nutritional deficiency or severe chronic disease)
Respiratory tract:
- Trachea: Open with scissors along the length — examine for: hemorrhage (LT virus, NDV), fibrinous or caseous exudate (MG + E. coli CRD complex), diphtheritic lesions (Fowl Pox wet form)
- Lungs: Normal (pink-red, spongy) or abnormal? Consolidation (grey, firm tissue = bacterial pneumonia), air sacculitis (white-grey fibrinous coating on air sac surfaces = E. coli colibacillosis, Aspergillus)
- Air sacs: Clear and transparent or thickened and cloudy? The “triangle of death” (pericarditis + perihepatitis + airsacculitis) is pathognomonic for colibacillosis
Cardiovascular:
- Heart size: Enlarged, rounded heart (right ventricular hypertrophy in ascites syndrome from Marek’s, or heavy metal toxicosis)
- Pericardium: Clear or fibrinous exudate? (Fibrinous pericarditis = E. coli or Mycoplasma synoviae systemic infection)
Liver:
- Color: Normal brown-red; pale yellow (fatty liver); bronze with friable texture (Fowl Typhoid); green-black (bile impregnation from bile duct obstruction); mottled with white nodules (Marek’s lymphoma, leukosis, aspergillosis)
- Hemorrhage: Capsule rupture and blood-filled abdominal cavity = Fatty Liver Hemorrhage Syndrome
Spleen:
- Normal: Small, dark red, bean-shaped
- Enlarged: Marek’s disease, leukosis, Fowl Typhoid, Fowl Cholera
- Mottled grey-white nodules: Marek’s lymphoma
Kidneys:
- Normal: Reddish-brown, three-lobed, embedded in the pelvis
- Pale and enlarged with urate deposits: Gout (from excess protein, calcium, or kidney damage); nephropathogenic IBV; calcium nephrosis from early high-calcium feeding
Gastrointestinal tract:
- Proventriculus: Hemorrhagic lesions in the glandular mucosa — pathognomonic for velogenic viscerotropic NDV
- Gizzard: Normal (muscular with green-grey content); open and examine for foreign bodies or erosion of the koilin layer (propionic acid toxicity, T-2 toxin from mycotoxin)
- Small intestine: Open with scissors — look for: roundworms (Ascaridia) in the lumen (visible with naked eye), hemorrhagic streaks (coccidiosis), necrotic plaques in the mucosa (Clostridium perfringens necrotic enteritis), tapeworm segments
- Ceca: Normal or hemorrhagic? Cecal hemorrhage = cecal coccidiosis (Eimeria tenella); cheesy cecal core = Histomonas meleagridis (blackhead)
Reproductive tract (in laying hens):
- Ovary: Normal follicular hierarchy (large yellow follicles in ordered size sequence) or abnormal? Regressed ovary (stress, disease); follicular rupture with free yolk in the abdomen (egg peritonitis)
- Oviduct: Open and examine — caseous material (E. coli salpingitis), impacted yolk material (impacted egg), thin mucosa (vitamin A deficiency), fibrin adhesions
Bursa of Fabricius:
- In pullets only (atrophies by week 12–16): Enlarged and edematous (acute Gumboro), or atrophied and smaller than expected for age (post-Gumboro immunosuppression)
Stage 5 — Building the Differential Diagnosis
After completing Stages 1–4, the diagnostic picture consists of:
- A set of flock-level observations (mortality rate, production changes, behavioral pattern)
- Individual bird clinical signs
- Production and management history for the previous 14 days
- Gross pathology findings from necropsy
The differential diagnosis is built by identifying the finding pattern that is most consistent with a known disease:
Pattern matching — the key differential combinations:
| Finding Combination | Primary Differentials |
|---|---|
| Sudden high mortality + proventricular hemorrhage + green diarrhea + torticollis | Velogenic Newcastle disease |
| Airsacculitis + pericarditis + perihepatitis (triangle of death) | Colibacillosis (E. coli) ± predisposing viral cause |
| Bursal edema or atrophy in young birds + depression + white diarrhea | Infectious Bursal Disease (Gumboro) |
| Peripheral nerve enlargement + unilateral lameness + visceral lymphoma | Marek’s Disease |
| Bronze, friable, enlarged liver + spleen enlargement + green-yellow diarrhea | Fatty Liver Hemorrhage Syndrome |
| Pale comb + pendulous abdomen + pericardial effusion + enlarged right ventricle | Ascites / Water Belly |
| Tracheal hemorrhage + gasping + rattling sound | Infectious Laryngotracheitis (ILT) |
| Egg drop + rough-shelled eggs + nephritis + kidney urate deposits | Infectious Bronchitis (nephropathogenic strain) |
| Bilateral facial swelling + mucopurulent nasal discharge + foul smell | Infectious Coryza (Avibacterium paragallinarum) |
| Bronze, friable enlarged liver + spleen enlargement + green-yellow diarrhea | Fowl Typhoid (Salmonella Gallinarum) |
| Intestinal coccidial lesions + blood-tinged droppings + mortality in young pullets | Coccidiosis (Eimeria spp.) |
| Bloody cecal content + cecal core | Cecal coccidiosis / Blackhead (Histomonas meleagridis) |
| Necrotic plaques in small intestinal mucosa + wet and bloody litter | Necrotic Enteritis (Clostridium perfringens) |
A provisional diagnosis is the combination of findings most consistent with the observed pattern. It is provisional because laboratory confirmation may revise it, but it is specific enough to drive an immediate management response.
The Decision Matrix: What to Do with the Diagnosis
A diagnosis is only valuable if it drives the right action in the right timeframe. The decision matrix converts the provisional diagnosis into a management response.
Immediate Actions (First 6 Hours)
If velogenic Newcastle disease is provisionally diagnosed:
- Implement immediate farm-wide lockdown — no movement of personnel, equipment, or birds out of the affected house
- Contact your veterinarian immediately — NDV is notifiable in Cameroon and Nigeria
- Administer emergency La Sota vaccination to all unaffected houses on the farm by spray or eye drop
- Begin supportive care (electrolytes + vitamins A, D, E, C in water) in the affected house
- Do not treat with antibiotics as a primary response — there is no antiviral treatment for NDV; antibiotics address only secondary bacterial infections
If E. coli colibacillosis is provisionally diagnosed:
- Collect fresh dead birds and submit for culture and sensitivity testing
- Begin empirical antibiotic treatment while awaiting sensitivity results if daily mortality exceeds 0.2%
- Identify and address the predisposing factor — elevated ammonia, waterline contamination, vaccination gap, concurrent viral infection
- Antibiotic treatment without addressing the predisposing factor will produce temporary improvement followed by relapse
If Marek’s Disease is provisionally diagnosed:
- No treatment available — Marek’s disease is a lifelong oncogenic viral infection
- Verify that Marek’s vaccination at day 1 hatchery was correctly administered and the cold chain was maintained
- Record the onset week and age of affected birds — early onset (weeks 6–10) suggests vaccine failure; late onset (weeks 18–30) is typical of field exposure
- Cull affected birds to prevent cannibalism targeting paralyzed birds; remove to reduce virus shed
If Gumboro (IBD) is provisionally diagnosed (in pullets):
- No specific treatment — supportive care with electrolytes, vitamins, and glucose in water
- Antibiotics for secondary E. coli infections if concurrent airsacculitis or peritonitis signs are present
- Review IBD vaccination timing relative to the maternal antibody profile — consider revising the vaccination protocol for the next flock
- Expect prolonged immunosuppression in recovered birds — plan for more vigilant monitoring of secondary disease events for the following 4–6 weeks
If Fatty Liver Hemorrhage Syndrome is provisionally diagnosed:
- This is a nutritional-metabolic condition, not infectious — no treatment or quarantine response needed
- Reduce ration energy density by 50–100 kcal/kg (reduce fat or oil supplementation)
- Increase choline (1 g/kg of ration) and vitamin E (40 IU/kg) — both have demonstrated protective effects against fatty liver pathology
- Ensure adequate methionine (0.72–0.78% of ration) — methionine deficiency impairs lipid export from hepatocytes
- Address overcrowding and heat stress if present — both independently elevate fatty liver risk
When to Call the Veterinarian: The Threshold Criteria
The farm diagnosis framework generates a provisional diagnosis and immediate actions. It does not replace veterinary diagnosis — it prepares the farm manager to communicate the clinical picture accurately when the veterinarian is contacted, enabling the veterinarian to provide more targeted guidance without an on-farm visit when that is not possible.
Call the veterinarian immediately when:
- Daily mortality exceeds 0.5% of the flock on any single day
- The flock-level clinical presentation does not match any of the differential patterns in Stage 5
- The provisional diagnosis suggests a notifiable disease (NDV, Marek’s with high early prevalence, Salmonella Gallinarum)
- A treatment has been initiated for 5 days without measurable improvement
- Multiple houses are simultaneously affected
- Egg production has dropped more than 20% in 5 days without a clear nutritional or management cause
When calling, provide: flock age in weeks, approximate number of affected birds, daily mortality for the previous 5 days, the findings from the clinical and necropsy examination, the vaccination history for the past 30 days, and any recent management changes. A veterinarian who receives this information can often make a remote provisional diagnosis and recommend treatment before they physically arrive on-farm.
Submitting Samples to the Diagnostic Laboratory: Getting Results That Help
Farm-level diagnosis is provisional. Laboratory diagnosis is confirmatory. The quality of the laboratory result depends entirely on sample quality and submission logistics.
Sample Collection Protocol
For bacteriology: Collect fresh tissue from recently dead birds (less than 4 hours post-mortem): liver, spleen, brain (where neurological signs are present), oviduct (where reproductive signs dominate), air sac swab (where airsacculitis is found). Use sterile swabs or sterile containers. Keep at 4°C (ice pack in an insulated bag — never freeze). Submit within 24 hours.
For virology (PCR or virus isolation): Collect trachea, lungs, spleen, brain, or cecal tonsil depending on the clinical syndrome, into virus transport medium (VTM) supplied by the laboratory. Keep at 4°C. Submit within 48 hours for PCR; within 24 hours for virus isolation.
For histopathology: Fix tissues in 10% neutral buffered formalin (10 parts formalin to 1 part tissue). Tissues can be submitted at ambient temperature once fixed. This is the most forgiving collection method and the most useful for Marek’s disease, leukosis, and any suspected tumoral condition.
For parasitology: Submit fresh fecal samples (10–20 grams from 20–30 birds) in a sealed container at 4°C. Do not use formalin for fecal samples intended for McMaster flotation — formalin kills the eggs but does not preserve them for counting. Submit within 48 hours.
Submission information to include: Farm name and location, species and age of birds, flock size, clinical signs, mortality rate and duration, vaccination history, and provisional diagnosis from farm-level assessment. The more specific and complete the submission information, the more focused the laboratory testing will be.
Summary
A farm diagnosis tool is not a replacement for veterinary expertise. It is the structured process that closes the gap between “something is wrong” and “I have a specific clinical picture to investigate and a provisional diagnosis to act on” — so that the time between disease onset and appropriate response is measured in hours rather than days.
The five stages — flock-level observation, individual bird examination, production and management history review, necropsy, and differential diagnosis — are not complex. They are sequential. They require attention, a consistent examination sequence, and the discipline not to stop at the first sign that suggests a hypothesis before the rest of the picture has been documented.
The farms that contain disease events, rather than being overwhelmed by them, are the farms where the diagnosis starts the moment the first abnormal bird is noticed, proceeds through all five stages before a treatment decision is made, and results in a veterinary contact with a complete clinical picture ready to communicate.
Disease events are not emergencies that paralyze management. They are diagnostic questions with a specific answer waiting to be found. Find the answer systematically. Every time.